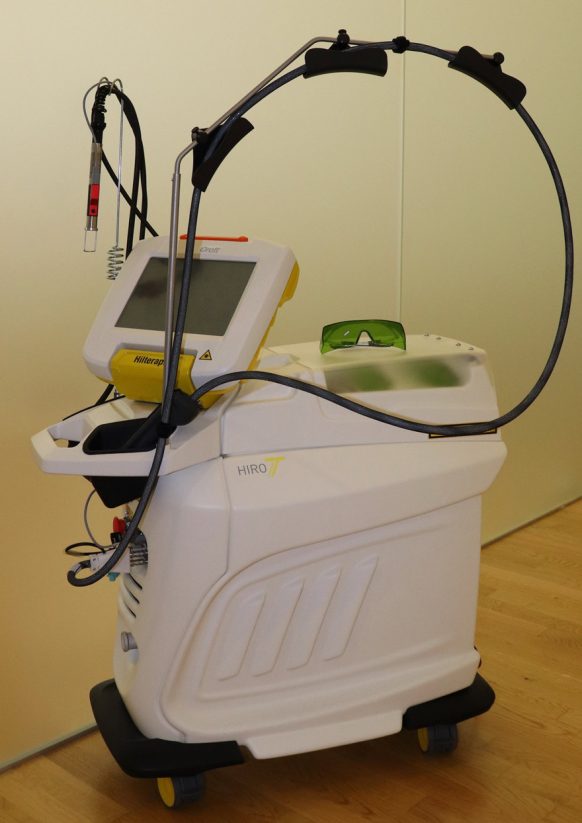
High-energy laser therapy has anti-inflammatory and analgesic effects. In addition to the pain-relieving effect, bio-stimulation causes rapid tissue regeneration and dissolution of bruises (hematomas).
High-energy, focused laser light stimulates blood flow in the treated tissue and improves metabolism. The cells stimulated in this way increase their metabolism and cell regeneration is stimulated. Inflammatory products and fluid accumulation are eliminated more quickly and healing processes are accelerated by increasing lymphatic and venous microcirculation.
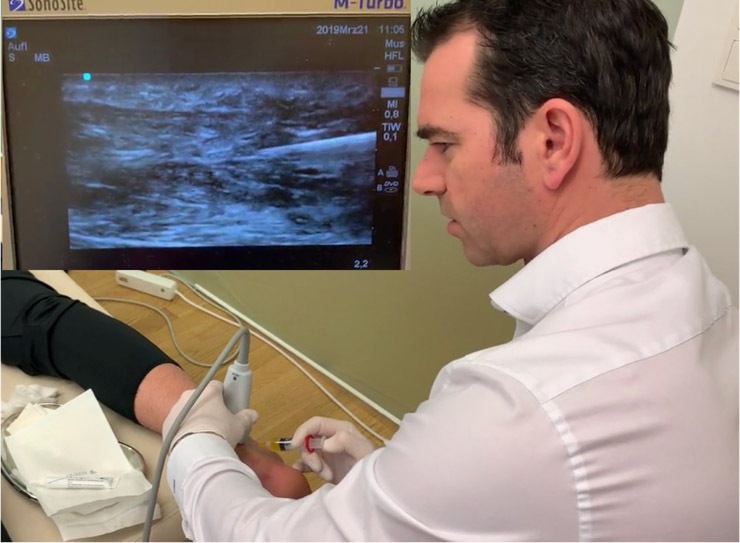
Furthermore, stimulation of endorphin release can be observed, which makes the laser highly suitable as a pain therapy for the treatment of inflammatory and traumatic changes of the musculoskeletal system, as they occur especially after operations or accidents. Especially after surgical interventions, the use of a high-energy laser leads to faster hematoma resolution and tissue regeneration, as well as pain reduction.